DBP3:UCLA
Contents
Introduction
What is traumatic brain injury?
Traumatic brain injury, often referred to as TBI, is most often an acute event that results in severe damage to portions of the brain. TBI results when the head suddenly and violently hits an object, or when an object pierces the skull and enters brain tissue. Symptoms of can be mild, moderate, or severe, depending on the extent of the damage to the brain. Common disabilities include cognitive deficits, sensory processing, communication, and behavior or mental health. Severe TBI may result in stupor where an individual can be aroused briefly by a strong stimulus (e.g. sharp pain); coma, where an individual is totally unconscious, unresponsive, unaware, and un-arousable; vegetative state, where an individual is unconscious and unaware of his or her surroundings, but continues to have a sleep-wake cycle and periods of alertness; and a persistent vegetative state, where an individual remains unresponsive for more than a month.
According to the CDC (United States Centers for Disease Control and Prevention), there are approximately 1.7 million people in the U.S. who suffer from a traumatic brain injury each year. 50,000 people die from TBI each year and 85,000 people suffer long term disabilities. In the U.S., more than 5.3 million people live with disabilities caused by TBI. Patients admitted to a hospital for TBI are included in this count, while those treated in an emergency room or doctor's office are not counted. The causes of TBI are diverse. The top three causes are: car accident, firearms and falls. Firearm injuries are often fatal: 9 out of 10 people die from such injuries. Young adults and the elderly are the age groups at highest risk for TBI. Along with a traumatic brain injury, persons are also susceptible to spinal cord injuries which is another type of traumatic injury that can result out of vehicle crashes, firearms and falls. Prevention of TBI is the best approach since there is no cure or way to reverse brain damage of this kind.
Mechanisms of TBI
Understanding the various mechanisms of TBI can be helpful for the development of robust and reliable computational algorithms for neuroimage data processing. These mechanisms are the highest causes of brain injury: Open head Injury, Closed Head Injury, Deceleration Injuries, Chemical/Toxic, Hypoxia, Tumors, Infections and Stroke.
1. Open Head Injury
* Results from bullet wounds, etc. * Largely focal damage * Penetration of the skull * Effects can be just as serious as closed brain injury
2. Closed Head Injury
* Resulting from a slip and fall, motor vehicle crashes, etc. * Focal damage and diffuse damage to axons * Effects tend to be broad (diffuse) * No penetration to the skull
3. Deceleration Injuries (Diffuse Axonal Injury) The skull is hard and inflexible while the brain is soft with the consistency of gelatin. The brain is encased inside the skull. During the movement of the skull through space (acceleration) and the rapid discontinuation of this action when the skull meets a stationary object (deceleration) causes the brain to move inside the skull. The brain moves at a different rate than the skull because it is soft. Different parts of the brain move at different speeds because of their relative lightness or heaviness. The differential movement of the skull and the brain when the head is struck results in direct brain injury, due to diffuse axonal shearing, contusion and brain swelling.
Diffuse axonal shearing: when the brain is slammed back and forth inside the skull it is alternately compressed and stretched because of the gelatinous consistency. The long, fragile axons of the neurons (single nerve cells in the brain and spinal cord) are also compressed and stretched. If the impact is strong enough, axons can be stretched until they are torn. This is called axonal shearing. When this happens, the neuron dies. After a severe brain injury, there is massive axonal shearing and neuron death.
4. Chemical/Toxic
* Also known as metabolic disorders * This occurs when harmful chemicals damage the neurons * Chemicals and toxins, e.g. insecticides, solvents, carbon monoxide poisoning, lead poisoning, etc.
5. Hypoxia (Lack of Oxygen)
* If the blood flow is depleted of oxygen, then irreversible brain injury can occur from anoxia (no oxygen) or hypoxia (reduced oxygen) * This condition may be caused by heart attacks, respiratory failure, drops in blood pressure and a low oxygen environment * This type of brain injury can result in severe cognitive and memory deficits
6. Tumors
* Tumors caused by cancer can grow on or over the brain * Tumors can cause brain injury by invading the spaces of the brain and causing direct damage * Damage can also result from pressure effects around an enlarged tumor * Surgical procedures to remove the tumor may also contribute to brain injury
7. Infections
* The brain and surrounding membranes are very prone to infections if the special blood-brain protective system is breached * Viruses and bacteria can cause serious and life-threatening diseases of the brain (encephalitis) and meninges (meningitis)
8. Stroke
* If blood flow is blocked through a cerebral vascular accident (stroke), cell death in the area deprived of blood will result * If there is bleeding in or over the brain (hemorrhage or hematoma) because of a tear in an artery or vein, loss of blood flow and injury to the brain tissue by the blood will also result in brain damage
In this DBP, we will be primarily concentrating on #'s 1, 2, and 3.
Neurological Concomitants of TBI
Following TBI, a cascade of neuroanatomical alterations initiate, with diffuse alterations in cortical structure peripheral to the point of injury but also distributed throughout the brain. Notably, there is ventricular enlargement and cortical thickness changes remote from the site of the TBI. White matter connectivity can be significantly altered with greatly reduced efficiency of signal transduction over affected pathways or complete cessation of inter-regional communication due to axonal damage. This can have profound effects on speech, motor, and cognitive processes. The extent of change is putatively related to the severity of TBI, location, subject age, and post-injury treatment, among other factors.
Challenges of TBI Neuroimaging
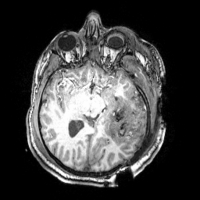
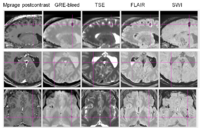
On anatomical MRI scans, TBI-related insults can appear as hyper-intensities, varying in magnitude and extent the degree to which tends to correlate with clinical symptoms. Additionally, in severe TBI, sections of skull, fractured during the injury or removed during surgical intervention, may not form a contiguous boundary enabling efficient digital removal of bone and other non-brain tissues, complicating tissue segmentation, regional parcellation, the measurement of ventricular size, cortical thickness, and other metrics. Computational algorithms require refinement to include constraints to account for TBI related signal alterations in anatomical scans; e.g. users may have to manually indicate regions encompassing the site of injury on the scans to guide local processing around the site and to reduce the weight of these regions on other, non-affected brain areas. Alternatively, probabilistic classifiers may need to include an extra classification for voxels whose tissue properties have been altered by TBI. This is particularly the case in diffusion weighted imaging (DWI) where the presence of TBI-related alterations in signal may reflect specific damage to white matter proximal to the lesion as well as long reaching effects along tracts to peripherally connected regions of cortex.
Project Goals and Specific Aims
Project Goals
An increasingly relevant means for the neurological assessment of traumatic brain injury (TBI) is with in vivo neuroimaging. However, standard automated image analysis methods are not robust with respect to the TBI-related changes in image contrast, changes in brain shape, cranial fractures, white matter fiber alterations, and other signatures of head injury. Multimodal quantification of brain insults and associating these with clinical and outcome metrics is a particular challenge. The emphasis in this DBP is placed on the feasibility of subject-specific analysis, as opposed to population-based averaging, to examine the influence of TBI on time-dependent alteration of gray and white matter integrity with accompanying change in clinical outcome variables to be used in subsequent TBI assessment. This DBP [1] seeks to:
1. Develop end-to-end processing approaches using the NA-MIC Kit to investigate alterations in cortical thickness, and subsequent ventricular and white matter changes in patients with TBI and in age-matched controls. Image processing will include segmentation of lesions, hemorrhage, edema, and other pathology relevant to TBI. Longitudinal changes will be assessed by registration and joint segmentation of baseline and follow-up data.
2. Develop robust workflows for diffusion weighted imaging (e.g. DTI, HARDI) datasets from TBI patients, by using the NA-MIC Kit and Slicer to obtain reliable and robust metrics of white matter pathology and of white matter changes due to therapy and/or recovery.
3. Using the NA-MIC Kit, cross-correlate multimodal metrics of cortical thickness, complexity, ventricular volume, and lesions from structural imaging and white matter fiber integrity from diffusion tensor imaging, with clinical outcome variables, i.e., time since injury, age, gender and other potential factors predictive of recovery.
Specific Aims
In this NA-MIC DBP, we seek to develop the means for guided and semi-automatic TBI analysis and quantification with a view toward assessing clinical improvement under the following Specific Aims:
Aim 1
How can multimodal assessment of altered brain anatomy speak directly to questions of brain plasticity and to secondary neuroanatomical effects of TBI?
We will develop end-to-end processing approaches using the NA-MIC Kit to investigate alterations in cortical thickness, subsequent ventricular, and white matter changes in patients with TBI and in age-matched controls.
Aim 2
Can multimodal workflows be developed to guide clinicians in the analysis and display of white matter fiber tract pathology that frequently accompanies brain insult?
In diffusion weighted imaging (e.g. DTI, HARDI) datasets from TBI patients, we will develop robust workflows using the NA-MIC Kit and Slicer to obtain reliable and robust metrics of white matter pathology.
Aim 3
How can multimodal metrics of TBI grey and white matter pathology be utilized to inform and guide clinical assessment?
Using the NA-MIC Kit, multimodal metrics of cortical thickness, complexity, and ventricular-volume from structural imaging and white matter fiber integrity from diffusion tensor imaging will be cross-correlated with clinical outcome variables, time since injury, age, gender and other potential factors predictive of recovery. We will emphasize the feasibility of subject-specific analysis, as opposed to population-based averaging, to examine the influence of TBI on time-dependent alteration of gray and white matter integrity with accompanying change in clinical outcome variables to be used in subsequent TBI assessment.
Use of NA-MIC Resources
Under this DBP, using sophisticated NA-MIC tools, we will develop end-to-end processing solutions by which to examine TBI neuroimaging data. The NA-MIC Kit encompasses a collection of tools for automated or semi-automated processing of medical imaging data. Notable is the Insight Toolkit (http://www.itk.org) for use in brain registration and segmentation via the 3D Slicer (http://www.slicer.org) software platform. These software tools may be linked to form data processing workflows that can process data via end-to-end solutions that may be shared with others, posted on websites, and used in training materials. They form an excellent platform for user-guided, patient-specific analysis, however, require additional development to inform the program about regions where TBI-related signal changes may necessitate alteration of model parameters or search volumes.
Case Analysis Goals
- Multimodal registration within and between scan sessions separated by ~6 months
- Computation of neuroanatomical measures of change per unit time in each case
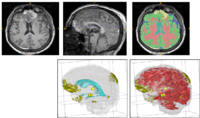
- Visualization of 3D models and their degree of change
- Quantification of alterations in ventricle and WM/GM volume, surface, cortical thickness, and other morphological metrics at time 1 and time 2
- Ability to quantify changes in diffusion local to the lesions as well as overall mean FA and fiber patterns between scan sessions
- Generation of a clinical report for each TBI patient. The clinician should have the ability to store such a report and use it in conjunction with their neurological assessments to gain insight about the case. It would be nice if that report could be generated not only in printer-friendly format but also in XML (or similar format) so that it can be read without much trouble into Matlab, R, or other secondary analysis frameworks or databases.
- Semi-automatic segmentation. Certain aspects of image segmentation segmentation may need to be user-guided (e.g. to conditionalize segmentation given the presence of a lesion), though in a way that is easy for clinicians to use. The user might point and click on an area exhibiting a bleed, or some other type of hypo-/hyperintesity. A boundary contour could then be found around that area, and the segmentation model would then be weighted by the presence of that area as some unique tissue type.
- Creation of population-based atlases from multiple TBI subjects or at least reference to standardized coordinate systems
Tasks
Software Requests
- The UCLA team would like to have Windows compilations of (1) the Longitudinal Lesion Comparison and (2) the Lesion Segmentation Applications Modules.
In Progress
In reverse chronological order:
- There is some interest in a macro capability to record selections for later playback
- Full brain fiber tractography
- NIFTI 4D file read/write, external gradient information importation, and a gradient table editor for DTI
- Better interoperability between LPS/RAS file organization in Slicer vs. vTK
- Ability to set direction cosines directly in Slicer volumes module
- Timed autosave functionality of scene files and other filetypes fundamental to Slicer (saved for several time steps)
- Welcome screen should be a pop-up window in the middle of screen that could be disabled
- Integration of volume render with slice displays (rendering set aside as an option)
- Import tools for DTIStudio and TrackVis tractography files
- Creating 3D ROIs using the edge detection routine
- Use of customizable toolbars for commonly used operations/features/modules/workflows/etc
- Volumes shouldn’t be loaded differently from “other data”
- Screen shot functionality shouldn’t force a re-render
- Being able to record video sequences (at least we couldn’t readily find this capability)
- NIFTI fMRI processing capability (3D+time)
Completed
- 2010-Dec-20. ABC module has been successfully compiled for Windows and tested (use Slicer nightly build for best results). Our thanks to Marcel and to the Utah team!
Data
- Need to obtain CT and PET for each example case (Jack Van Horn, UCLA TBI team)
Results
Sample Data Sets
The following cases represent severe instances of TBI scanned using MRI brain imaging techniques. The (zipped) anatomical data files are in NIFTI format while DWI files are in Nrrd format. Additional data from PET and from CT will be forthcoming for these cases, as well.
- File:TBI Patient1 nrrd3.zip
- File:TBI Patient2 nrrd2.zip
- File:Patient3 DTI nrrd files.zip
- File:Patient1 UCLA 3T.zip
- File:Patient2 UCLA 3T.zip
- File:Patient3 UCLA 3T.zip
- File:UCLA 1 5T.zip
- File:UCLA 3T.zip
Sample Slicer Results
The following PDF contains a presentation prepared by Dr. Guido Gerig which showcases some example results on the above TBI data sets obtained using existing and newly developed Slicer processing modules.
Outreach
- TBI DBP Presentation at NA-MIC AHM (January 2011; Jack Van Horn)
- TBI Cases TBI Registration Case Library
- Develop comprehensive tutorial/how-to guide
- Design user friendly TBI workflow interface for Slicer
- Presentations/posters at OHBM, SFN, and other (inter)national meetings in year 2
- Hands-on teaching event for the DBP scientific community for year 3
- Peer reviewed publications
Investigators
- John Darrell Van Horn (UCLA) - DBP PI
- Andrei Irimia (UCLA) - DBP Engineer
- Micah Chambers (UCLA)
- Arthur W. Toga (UCLA)
- David Hovda (UCLA)
- Paul Vespa (UCLA)
- Jeffry Alger (UCLA)
- Guido Gerig (UTAH)
- Stephen Aylward (Kitware)
- Danielle Pace (Kitware)