Difference between revisions of "Events:HST-563-March2008"
| (39 intermediate revisions by 2 users not shown) | |||
| Line 1: | Line 1: | ||
| + | =Lecturer= | ||
| + | Nobuhiko Hata, PhD ([http://www.spl.harvard.edu/pages/People/noby Dr. Hata's personal web page]) | ||
| + | |||
| + | Assistant Professor of Radiology, Harvard Medical School | ||
| + | |||
| + | Director, Surgical Navigation and Robotics Laboratory (www.snrlab.org) | ||
| + | |||
| + | |||
=Lab date/time/location= | =Lab date/time/location= | ||
| − | *March 19, 2008 | + | *3:00- 5:00pm, March 19, 2008 |
| − | * | + | *Direction http://www.spl.harvard.edu/pages/Directions |
| + | |||
| + | |||
| + | ==Background:== | ||
| − | + | [[Image:robot.png|200px]] | |
| + | [[Image:slicer.png|200px]] | ||
| − | == | + | In comparison to other medical imaging modalities, magnetic resonance imaging (MRI) has clear advantages in its volumetric scanning capabilities, tissue discrimination and the detailed delineation of anatomic features. Additionally, MR imaging has unique potential capabilities for functional physiologic imaging and temperature mapping. These features of MR imaging motivated the development of intraoperative MR imaging (IMRI) for guidance of biopsy, thermal ablation and other surgical procedures. The major application of IMRI has been neurosurgical cases, including biopsy, drainage and tumor ablation. Other applications include liver biopsy and sinus endoscopic surgery. |
| + | |||
| + | There are many benefits in using pre-operatively obtained MRI as part of an analysis of imagery from IMRI. For example, IMRI has some limitations in its imaging capability in comparison to pre-operative MRI from conventional diagnostic MR scanner, since requirements for interventional use (for example, the use of surface coils for good access) have some impact on the imaging capability. After performing a registration that determines the proper spatial relationship between the pre-operative MRI and IMRI, one could compare and determine whether changes in tissue structure have occurred. For instance, this would be extremely useful in evaluating the extent of tumor. | ||
| + | |||
| + | We can further appreciate the benefit of pre-operative image, if we can co-register imagery from other modalities than MRI. Currently, we can register computed tomography (CT), T1- and T2-weighted MRI: magnetic resonance angiography (MRA), single photon emission computed tomography (SPECT). Incorporation of these images can provide information that can not be deduced from regular MRI. | ||
| + | In general, utilizing pre- and intra-operative image registration would allow a surgeon to more precisely identify and avoid critical structures and more accurately locate pathological tissues during a procedure. | ||
| + | |||
| + | In this laboratory course, we will present our approach to register pre-operative image to intra-operative MRI and use co-registered images to navigate neurosurgeries. We will first outline the registration method through maximization of mutual information. Then, the comprehensive accuracy study of the registration and clinical application of the method are introduced. In the clinical application section, we will introduce our engineering and computational setup to achieve online and near real-time registration and navigation in an inerventional MRI scanner. | ||
| + | An example scenario | ||
| + | |||
| + | ===Recommended reading before the class=== | ||
| + | The following papers describe a number of IMRI applications currently under development at the Surgical Planning Laboratory. Please read the paper on neurosurgery and be familiar with the other applications. | ||
| + | |||
| + | '''Image-guided Neurosurgery at Brigham and Women’s Hospital''' | ||
| + | http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=294 | ||
| + | |||
| + | '''MR-guided prostate interventions''' | ||
| + | http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1225 | ||
| + | |||
| + | '''Current status and future potential of MRI-guided focused ultrasound surgery''' | ||
| + | http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1244 | ||
| + | |||
| + | '''MRI-guided cryotherapy''' | ||
| + | http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1247 | ||
| + | |||
| + | ===Recommended exercise before the class=== | ||
| − | + | If you are interested in learning how we process pre-operative images in preparation for MRI-guided therapy, download the free software slicer following the instructions in the "Slicer 101" page below. | |
| − | + | http://wiki.na-mic.org/Wiki/index.php/Slicer:Workshops:User_Training_101 | |
| − | |||
| − | + | Among the courses available in the web page, we suggest you take the following topics.. | |
| + | *Data Loading and Visualization | ||
| + | *Data Saving | ||
| + | *Manual Segmentation | ||
| + | *Level-Set Segmentation | ||
| + | *Automatic Brain Segmentation | ||
| + | *Registration | ||
| − | + | ==On the day of the lab....== | |
| − | |||
| − | + | ===Introduction=== | |
| + | We will present the overview of the MRI-guided therapy and technologies involved in it. | ||
| + | ===Pre-operative diagnostic imaging=== | ||
| + | *fMRI, CT, MRI, DT-MRI, PET, CT | ||
| − | = | + | ===Surgical Planning=== |
| + | *preoperative imaging | ||
| + | *registration | ||
| + | *planning | ||
| − | + | ===Surgical Navigation=== | |
| − | + | *Patient-to-image registration | |
| + | Q. What is the patient-to-image registration? What kind of mathematical process is involved in the patient-to-image registration? | ||
| + | Q. What is Target Registration Error, Fiducial Registration Error, and Fiducial Localization error? | ||
| + | [[media:west1.zip]] | ||
| − | + | *Tracking device (optical and EM) | |
| − | + | *Guidance | |
| − | + | ===MRI-guided Therapy=== | |
| + | *What if we can take intra-operative image (demo) | ||
| − | + | Q. What is the difference between pre-operative image guided therapy and intra-operative image guided therapy? | |
| + | Q. How would you solve the problem that intra-operative MRI has inherently less quality than pre-operative images? | ||
| + | Q. What are the main clinical applications in MRI-guided therapy? | ||
| − | + | ==Homework problems== | |
| − | == | ||
| − | + | ===Problems we address in the demo=== | |
| − | + | #What is the patient-to-image registration? What kind of mathematical process is involved in the patient-to-image registration? | |
| + | #What is Target Registration Error, Fiducial Registration Error, and Fiducial Localization error? | ||
| + | #What is the difference between pre-operative image guided therapy and intra-operative image guided therapy? | ||
| + | #What is the benefit of MRI-guided intra-operative image guided therapy? | ||
| + | #How would you solve the problem that intra-operative MRI has inherently less quality than pre-operative images? | ||
| + | #What are the main clinical applications in MRI-guided therapy? | ||
| − | + | ===Open questions=== | |
| + | #What is the benefit of medical imaging for guiding and navigating surgery? | ||
| + | #What are the technologies involved in image guided therapy? List and briefly describe them in the order of workflow. | ||
| + | #From PubMed, find three interesting paper on MRI-guided therapy and summarize them. (Hint: the review papers on this topic can be found in the Feb 2008 issue of Journal Magnetic Resonance Imaging) | ||
| + | #What do you think is an unchallenged clinical target in MRI-guided therapy? (Hint: moving organs, soft tissue organs, tubular organs). Specify needs in the treatment and benefit of using MRI for guidance and monitoring. | ||
Latest revision as of 03:31, 19 March 2008
Home < Events:HST-563-March2008Contents
Lecturer
Nobuhiko Hata, PhD (Dr. Hata's personal web page)
Assistant Professor of Radiology, Harvard Medical School
Director, Surgical Navigation and Robotics Laboratory (www.snrlab.org)
Lab date/time/location
- 3:00- 5:00pm, March 19, 2008
- Direction http://www.spl.harvard.edu/pages/Directions
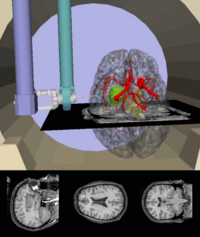
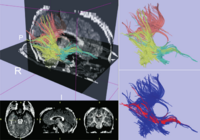
Background:
In comparison to other medical imaging modalities, magnetic resonance imaging (MRI) has clear advantages in its volumetric scanning capabilities, tissue discrimination and the detailed delineation of anatomic features. Additionally, MR imaging has unique potential capabilities for functional physiologic imaging and temperature mapping. These features of MR imaging motivated the development of intraoperative MR imaging (IMRI) for guidance of biopsy, thermal ablation and other surgical procedures. The major application of IMRI has been neurosurgical cases, including biopsy, drainage and tumor ablation. Other applications include liver biopsy and sinus endoscopic surgery.
There are many benefits in using pre-operatively obtained MRI as part of an analysis of imagery from IMRI. For example, IMRI has some limitations in its imaging capability in comparison to pre-operative MRI from conventional diagnostic MR scanner, since requirements for interventional use (for example, the use of surface coils for good access) have some impact on the imaging capability. After performing a registration that determines the proper spatial relationship between the pre-operative MRI and IMRI, one could compare and determine whether changes in tissue structure have occurred. For instance, this would be extremely useful in evaluating the extent of tumor.
We can further appreciate the benefit of pre-operative image, if we can co-register imagery from other modalities than MRI. Currently, we can register computed tomography (CT), T1- and T2-weighted MRI: magnetic resonance angiography (MRA), single photon emission computed tomography (SPECT). Incorporation of these images can provide information that can not be deduced from regular MRI. In general, utilizing pre- and intra-operative image registration would allow a surgeon to more precisely identify and avoid critical structures and more accurately locate pathological tissues during a procedure.
In this laboratory course, we will present our approach to register pre-operative image to intra-operative MRI and use co-registered images to navigate neurosurgeries. We will first outline the registration method through maximization of mutual information. Then, the comprehensive accuracy study of the registration and clinical application of the method are introduced. In the clinical application section, we will introduce our engineering and computational setup to achieve online and near real-time registration and navigation in an inerventional MRI scanner. An example scenario
Recommended reading before the class
The following papers describe a number of IMRI applications currently under development at the Surgical Planning Laboratory. Please read the paper on neurosurgery and be familiar with the other applications.
Image-guided Neurosurgery at Brigham and Women’s Hospital http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=294
MR-guided prostate interventions http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1225
Current status and future potential of MRI-guided focused ultrasound surgery http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1244
MRI-guided cryotherapy http://www.spl.harvard.edu/pages/Special:PubDB_View?dspaceid=1247
Recommended exercise before the class
If you are interested in learning how we process pre-operative images in preparation for MRI-guided therapy, download the free software slicer following the instructions in the "Slicer 101" page below. http://wiki.na-mic.org/Wiki/index.php/Slicer:Workshops:User_Training_101
Among the courses available in the web page, we suggest you take the following topics..
- Data Loading and Visualization
- Data Saving
- Manual Segmentation
- Level-Set Segmentation
- Automatic Brain Segmentation
- Registration
On the day of the lab....
Introduction
We will present the overview of the MRI-guided therapy and technologies involved in it.
Pre-operative diagnostic imaging
- fMRI, CT, MRI, DT-MRI, PET, CT
Surgical Planning
- preoperative imaging
- registration
- planning
- Patient-to-image registration
Q. What is the patient-to-image registration? What kind of mathematical process is involved in the patient-to-image registration? Q. What is Target Registration Error, Fiducial Registration Error, and Fiducial Localization error?
- Tracking device (optical and EM)
- Guidance
MRI-guided Therapy
- What if we can take intra-operative image (demo)
Q. What is the difference between pre-operative image guided therapy and intra-operative image guided therapy? Q. How would you solve the problem that intra-operative MRI has inherently less quality than pre-operative images? Q. What are the main clinical applications in MRI-guided therapy?
Homework problems
Problems we address in the demo
- What is the patient-to-image registration? What kind of mathematical process is involved in the patient-to-image registration?
- What is Target Registration Error, Fiducial Registration Error, and Fiducial Localization error?
- What is the difference between pre-operative image guided therapy and intra-operative image guided therapy?
- What is the benefit of MRI-guided intra-operative image guided therapy?
- How would you solve the problem that intra-operative MRI has inherently less quality than pre-operative images?
- What are the main clinical applications in MRI-guided therapy?
Open questions
- What is the benefit of medical imaging for guiding and navigating surgery?
- What are the technologies involved in image guided therapy? List and briefly describe them in the order of workflow.
- From PubMed, find three interesting paper on MRI-guided therapy and summarize them. (Hint: the review papers on this topic can be found in the Feb 2008 issue of Journal Magnetic Resonance Imaging)
- What do you think is an unchallenged clinical target in MRI-guided therapy? (Hint: moving organs, soft tissue organs, tubular organs). Specify needs in the treatment and benefit of using MRI for guidance and monitoring.