2012 Summer Project Week:SemiAutomatedAirwaySegmentationfrom0.64mmLungCTDatasets
Key Investigators
- University College Cork: Padraig Cantillon-Murphy, Pietro Nardelli
- HMS/HSDM: Raul San Jose Estepar
Objective
We are currently developing a system for endoscopic lung biopsy which would allow access to peripheral nodules using electromagnetic steering by means of external coils. The goal of the project is to steer a catheter inside the lung using an electromagnetic field (provided by 3 electromagnetic coils) and to couple this electromagnetic navigation system with real-time image registration so that the physician can see a 3D reconstruction of where he is in the airway by means of a virtual endoscopy system (registered to a prior CT).
Approach, Plan
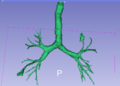
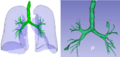
For the virtual endoscopy system we are using 3D Slicer to implement a new tool that should allow the physician to have a fast 3D reconstruction of the airway and to move inside it following the catheter. The idea for the tool is to firstly develop an element of semi-automatic segmentation improving the already available Slicer’s Simple Region Growing Module in order to obtain a new Adaptive Threshold Region Growing Module capable of automatic increment. Then, by choosing the right threshold to reconstruct the airway as well as possible and to avoid leakage problems: for this purpose, we are planning to follow the Kiraly’s method [1], which seems a good trade-off between complexity and segmentation’s capability. In this way, we think to be able to obtain a first non-complete but sufficient for the most of the times segmentation and reconstruction of the airway, Once the airway has been firstly segmented and reconstructed with the method above, the goal is to allow the physician to select the Region of Interest (ROI) (s)he wants to reach (such as a nodule inside a peripheral branch), and to implement a centerline extraction of the reconstructed airway, followed by a path decision, in order to obtain the right way to get the ROI: in this case, the Centerline Extraction Module developed by Estepar et al. for Airway Inspector (based on Slicer 2.8) [2] might be very helpful and we think to extend it to the new Slicer 4. As the last segmentation part, we are planning to add (if possible) some new method to the Editor module in order to allow the physician, if necessary, to add and see new or existing branches of the airway, which the automatic segmentation can miss. The idea here is to allow the physician to improve the automatic segmentation described above for the purposes of having an optimized path to get to ROIs in deepest part of the lung. Once the airway’s segmentation has been obtained and the lung has been reconstructed, we are planning to use (and possibly improve) the Slicer's Endoscopy and IGT Modules in order to move through the airway and to recognize and follow the catheter inside the lung. We have a very nice collaboration in Cork with some interventional pulmonologists in the area of guidance for lung biopsy in cancer patients and the datasets we are using were generated by a 64-GE MEDICAL SYSTEM scanner at Cork University Hospital, with 2mm of slice thickness and a standard convolution kernel. We have also available the CT datasets which were used during EXACT 2009 and are freely available, as a benchmark for our approach against others existing .
Progress
CLI Module for Airway Segmentation created, with quite good results (comparable with other team's results)
Delivery Mechanism
This work will be delivered to the NA-MIC Kit as a (please select the appropriate options by noting YES against them below)
- ITK Module
- Slicer Module
- Built-in - No
- Extension -- commandline - Yes
- Extension -- loadable
- Other (Please specify)
References
1. Kiraly AP, Higgings WE, McLennan G, Hoffman EA, McLennan G, Reinhardt JM. Three-dimensional human airway segmentation methods for clinical virtual bronchoscopy. Acad Radiol 2002;9:1153-1168.
2. San Jose Estepar R, Washko GG, Silverman EK, Reilly JJ, Kikinis R, Westin CF. Airway inspector: An open source application for lung morphometry. In First International Workshop on Pulmonary Image Processing. New York City, USA, 2008;293-302.